Stem Cell Therapy for Sports Rehabilitation
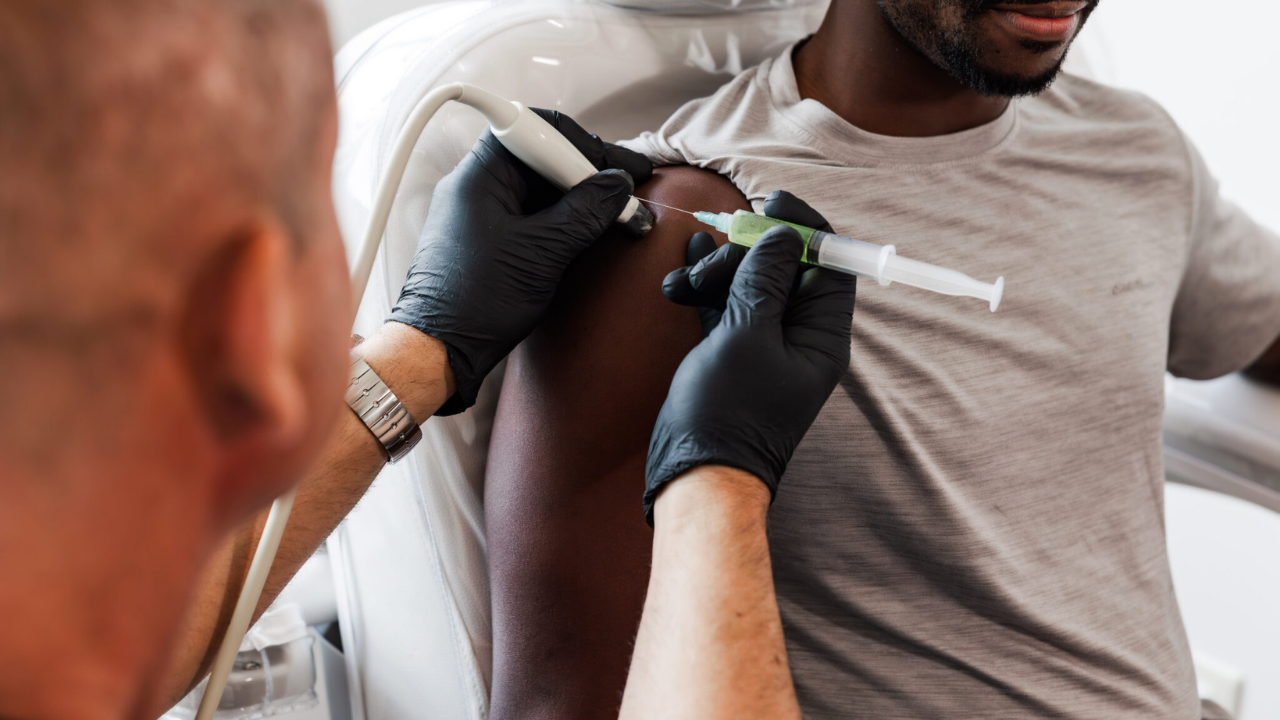
Stem Cell Therapy for Sports Rehabilitation
Stem cell therapy is an innovative rehabilitation method that accelerates tissue repair, reduces inflammation, and helps athletes return to peak performance faster and more safely.
Sports injuries are among the most common challenges faced by professional athletes, recreational athletes, and physically active individuals. Intense training, repetitive motion, sudden trauma, poor biomechanics, inadequate recovery, and overuse can place excessive stress on muscles, tendons, ligaments, cartilage, bones, and joints. As a result, athletes may experience muscle tears, ligament sprains, tendon injuries, cartilage damage, joint inflammation, chronic pain, reduced mobility, and delayed return to sport.
The human body has a natural ability to repair injured tissues, but some sports injuries heal slowly or incompletely because of limited blood supply, repeated stress, scar tissue formation, inflammation, or premature return to activity. Tendons, ligaments, cartilage, and certain joint structures are especially vulnerable to prolonged recovery. When symptoms persist despite rest, physical therapy, medications, injections, or surgery, regenerative medicine may be considered as a supportive option in selected patients.
Stem cell therapy for sports injuries is being explored as a regenerative approach that may help modulate inflammation, support tissue repair signaling, improve cellular communication, and enhance the biological environment around injured tissues. Mesenchymal stem cells, platelet-rich plasma, exosomes, and growth factor-supported protocols may be used in selected cases to support recovery, mobility, and long-term tissue health.
Stemcell Consultancy provides personalized regenerative treatment planning for eligible athletes and active individuals with sports-related injuries. The goal is to support safe recovery, reduce pain burden, improve movement quality, and help patients return to activity through medically supervised protocols, realistic expectations, and structured rehabilitation support.
What Are Sports Injuries?
Sports injuries are injuries that occur during exercise, training, competition, physical activity, or repetitive athletic movement. They may develop suddenly after trauma or gradually due to overuse. The type of injury depends on the sport, movement pattern, training load, age, flexibility, strength, recovery habits, footwear, equipment, and underlying biomechanics.
Sports injuries may affect:
- Muscles
- Tendons
- Ligaments
- Cartilage
- Meniscus tissue
- Joint capsules
- Bursae
- Bones
- Nerves
- Fascia and connective tissue
Some injuries improve with conservative care, while others require imaging, specialist evaluation, injections, surgery, or long-term rehabilitation. A correct diagnosis is essential before any regenerative therapy is considered.
Acute Sports Injuries vs. Overuse Injuries
Sports injuries are commonly divided into acute injuries and overuse injuries. Understanding the difference helps determine the right treatment strategy.
Acute Sports Injuries
Acute injuries happen suddenly, usually after a fall, collision, twist, direct blow, sprint, jump, or sudden overload. Examples include ankle sprains, ACL injuries, hamstring tears, shoulder dislocations, fractures, meniscus tears, or muscle strains.
Acute symptoms may include sudden pain, swelling, bruising, reduced movement, instability, inability to bear weight, or loss of strength. Some acute injuries require urgent medical care, especially when fracture, dislocation, tendon rupture, or severe ligament injury is suspected.
Overuse Sports Injuries
Overuse injuries develop gradually when tissues are exposed to repeated stress without enough recovery time. They are common in runners, tennis players, golfers, swimmers, basketball players, football players, martial artists, weightlifters, and endurance athletes.
Examples include tendinopathy, stress reactions, shin splints, tennis elbow, golfer’s elbow, rotator cuff irritation, patellar tendinopathy, Achilles tendinopathy, bursitis, cartilage irritation, and chronic joint inflammation.
Overuse injuries often require load management, rehabilitation, biomechanical correction, and gradual return to sport. Regenerative therapy may be considered in selected chronic cases when standard recovery is insufficient.
Common Types of Sports Injuries
Sports injuries vary widely depending on the tissue involved. Each injury type requires a different diagnostic and rehabilitation approach.
Muscle Injuries and Tears
Muscle injuries may occur during sprinting, jumping, lifting, sudden acceleration, or eccentric loading. Hamstrings, quadriceps, calves, adductors, and shoulder muscles are commonly affected.
Mild muscle strains may heal with rest and rehabilitation. More severe tears may cause bruising, weakness, swelling, and prolonged recovery. Regenerative therapy may be discussed in selected cases to support tissue repair signaling and reduce inflammation during recovery.
Tendon Injuries
Tendons connect muscles to bones. They are exposed to high loads and often have limited blood supply, which can slow healing. Tendon injuries may include tendinopathy, partial tears, chronic tendon irritation, or tendon rupture.
Common tendon conditions include Achilles tendinopathy, patellar tendinopathy, rotator cuff tendinopathy, tennis elbow, golfer’s elbow, and hamstring tendinopathy. Treatment often requires load management, strengthening, and gradual return to sport.
Ligament Injuries
Ligaments connect bones and provide joint stability. Sports-related ligament injuries may occur during twisting, landing, cutting, collision, or sudden changes in direction.
Common examples include ACL, MCL, PCL, LCL, ankle ligament sprains, shoulder ligament injuries, and wrist ligament injuries. Severe ligament injuries may require surgical evaluation, especially when instability is present.
Cartilage and Meniscus Injuries
Cartilage allows smooth joint movement, while the meniscus helps absorb shock and stabilize the knee. These tissues have limited healing capacity. Athletes may develop cartilage lesions, meniscus tears, joint degeneration, or early osteoarthritis after trauma or repetitive stress.
Regenerative therapy may be considered in selected mild to moderate cases to support inflammation regulation and joint environment health. Advanced cartilage loss or mechanical locking may require orthopedic evaluation.
Joint Inflammation and Bursitis
Repeated friction, impact, or poor mechanics can inflame joint structures and bursae. Shoulder bursitis, hip bursitis, knee bursitis, and elbow bursitis are common in athletes.
Infection must be ruled out when swelling, redness, warmth, fever, or severe tenderness is present. Regenerative therapy should not be performed when infection is suspected.
Post-Surgical Sports Recovery
Some athletes explore regenerative therapy after orthopedic surgery to support tissue healing, inflammation control, and rehabilitation. This should always be coordinated with the surgeon and rehabilitation team to avoid interfering with surgical recovery.
How Are Sports Injuries Diagnosed?
A proper diagnosis is essential before treatment planning. Pain location alone is not enough because different injuries can cause similar symptoms. For example, knee pain may come from a ligament injury, meniscus tear, cartilage damage, tendon irritation, bursitis, or referred pain from the hip or spine.
Diagnostic evaluation may include:
- Detailed injury history
- Sport and training load analysis
- Physical examination
- Range of motion testing
- Strength and stability assessment
- Biomechanical and gait evaluation
- Functional movement testing
- Ultrasound for tendon, ligament, or soft tissue assessment
- MRI for cartilage, meniscus, ligament, tendon, or muscle injuries
- X-ray when fracture, arthritis, or alignment problems are suspected
- CT scan in selected bone or complex joint injuries
- Laboratory tests when inflammatory disease or infection is suspected
Imaging is especially important when symptoms are severe, persistent, recurrent, or associated with instability, locking, weakness, or inability to return to sport.
When Should a Sports Injury Be Taken Seriously?
Some sports injuries require urgent medical evaluation. Athletes should seek prompt care if they experience:
- Severe pain after trauma
- Inability to bear weight
- Visible deformity
- Suspected fracture or dislocation
- Rapid swelling after injury
- Joint locking or inability to fully move the joint
- Severe instability or giving way
- Sudden loss of strength
- Numbness, tingling, or nerve symptoms
- Fever, redness, warmth, or signs of infection
- Persistent pain despite rest and rehabilitation
- Repeated injury in the same area
Regenerative therapy should not delay urgent orthopedic care when a serious injury is suspected.
Conventional Treatment Options for Sports Injuries
Standard sports injury treatment depends on injury type, severity, tissue involved, athlete goals, and competition demands. Many injuries improve with a structured conservative plan.
Common treatment options may include:
- Rest and activity modification
- Ice or heat depending on injury stage
- Compression and elevation for swelling control
- Nonsteroidal anti-inflammatory medications when appropriate
- Physical therapy
- Progressive strengthening
- Mobility and flexibility training
- Neuromuscular control exercises
- Balance and proprioception training
- Sport-specific rehabilitation
- Bracing, taping, or orthotics in selected cases
- Corticosteroid injections in selected inflammatory conditions
- PRP injections in selected tendon or joint conditions
- Surgical repair or reconstruction for severe structural injuries
Conventional care remains important even when regenerative therapy is considered. Tissue healing requires correct loading, movement quality, recovery time, and gradual return to sport.
Limitations of Traditional Sports Injury Treatments
Traditional treatments can be effective, but some athletes continue to experience pain, weakness, stiffness, or recurring injury. This may happen when inflammation persists, tissue quality is reduced, biomechanics are poor, or return to sport occurs too early.
Common limitations may include:
- Rest may reduce symptoms but does not always rebuild tissue strength.
- Pain medications may mask symptoms without correcting the underlying injury.
- Physical therapy requires consistency and may take time to restore full function.
- Corticosteroid injections may reduce inflammation but are not always suitable for repeated use around tendons.
- Surgery may be necessary in selected cases but involves downtime, recovery, and rehabilitation.
- Returning to sport too early may increase reinjury risk.
Regenerative medicine may be explored in selected cases to support the biological side of recovery while rehabilitation addresses strength, mobility, mechanics, and performance readiness.
What Makes Stem Cell Therapy Relevant for Sports Injuries?
Stem cell therapy is based on supporting the body’s biological repair processes. Mesenchymal stem cells, also known as MSCs, are being studied because they can release growth factors, cytokines, extracellular vesicles, and other signaling molecules that may influence inflammation, tissue repair, immune balance, and cellular communication.
In sports medicine, MSC-based regenerative protocols may help support:
- Inflammation modulation
- Tissue repair signaling
- Collagen remodeling support
- Cellular communication in injured tissues
- Soft tissue healing environment
- Joint microenvironment support
- Recovery when combined with rehabilitation
Stem cell therapy should not be described as a guaranteed cure, a guaranteed way to regenerate cartilage, or a guaranteed method to return to sport faster. Outcomes depend on diagnosis, injury severity, tissue quality, athlete health, rehabilitation compliance, training load, and time from injury.
How Stem Cells May Work in the Body for Sports Recovery
Stem cells may support sports injury recovery through several biological mechanisms. These effects should be understood as potential supportive mechanisms rather than guaranteed outcomes.
1. Inflammation Modulation
Inflammation is part of the healing process, but excessive or chronic inflammation can delay recovery and contribute to pain. MSC-related signaling may help regulate inflammatory pathways in selected tissue environments.
2. Tissue Repair Signaling
MSCs may release molecules that support repair-related activity in tendons, ligaments, muscles, cartilage, and connective tissues. This may help create a more favorable environment for recovery.
3. Collagen and Extracellular Matrix Support
Tendons and ligaments depend heavily on collagen organization. Regenerative signaling may support collagen remodeling and tissue quality when combined with appropriate loading and rehabilitation.
4. Cellular Communication
MSCs and exosomes may influence how cells communicate during healing. Improved cellular signaling may support coordination of repair processes in injured tissues.
5. Joint Environment Support
In cartilage or joint-related sports injuries, regenerative therapy may help support synovial balance, inflammation control, and the biological environment inside or around the joint.
The Role of PRP, Exosomes, and Growth Factors
Sports injury protocols may include PRP, exosomes, or growth factor-supported approaches depending on the injury type and medical suitability.
Platelet-Rich Plasma
PRP is prepared from the patient’s own blood and contains concentrated platelets and growth factors. It may be considered for selected tendon injuries, ligament sprains, muscle injuries, and mild to moderate joint degeneration.
Exosomes
Exosomes are extracellular vesicles involved in cell-to-cell communication. They are being studied for their potential role in inflammation regulation, repair signaling, and tissue communication. Their regulatory status varies by country, and patients should ask about product source, sterility, safety testing, and clinical evidence.
Growth Factors
Growth factors are biological molecules that may influence tissue repair, collagen remodeling, and healing activity. They may be used as part of selected regenerative protocols depending on diagnosis and treatment goals.
These supportive options are not necessary for every athlete. The treatment plan should be based on the injury type, severity, imaging findings, competition goals, safety profile, and rehabilitation plan.
How Stem Cell Therapy May Help Different Sports Injuries
Muscle Tears and Strains
Muscle injuries may benefit from treatment strategies that reduce inflammation and support organized repair. Regenerative therapy may be considered in selected cases to support healing signals, especially when recovery is delayed or reinjury risk is high.
Tendon and Ligament Injuries
Tendons and ligaments often heal slowly due to limited blood supply. MSC, PRP, or exosome-supported protocols may be considered in selected chronic or partial injuries to support collagen remodeling and tissue repair signaling.
Cartilage Damage and Joint Degeneration
Cartilage has limited natural healing capacity. Regenerative therapy may support the joint environment in selected mild to moderate cases, but complete cartilage regrowth cannot be guaranteed. Advanced cartilage loss may require orthopedic evaluation.
Overuse Injuries
Overuse injuries usually require load management, biomechanics correction, and gradual strengthening. Regenerative therapy may be considered as supportive care when chronic inflammation or tissue irritation persists despite rehabilitation.
Post-Surgical Recovery
Regenerative protocols may be discussed in selected post-surgical cases to support tissue healing and recovery, but timing must be coordinated with the orthopedic surgeon. Stem cell therapy should not replace proper surgical rehabilitation.
The Stemcell Consultancy Approach to Sports Rehabilitation
At Stemcell Consultancy, treatment protocols are personalized according to the athlete’s diagnosis, injury severity, imaging findings, performance goals, medical history, training demands, and return-to-sport timeline. The approach combines regenerative medicine with structured rehabilitation planning.
Depending on the patient’s suitability, protocols may include:
- Mesenchymal stem cells
- Umbilical cord-derived allogeneic MSCs
- PRP-supported therapy
- Exosome-supported protocols
- Regenerative growth factor support
- Image-guided application planning in selected cases
- Post-treatment rehabilitation and performance guidance
The goal is not only to reduce pain but also to support tissue quality, movement control, strength, and long-term resilience.
Step-by-Step Sports Stem Cell Treatment Process
Step 1: Initial Evaluation
The process begins with a detailed assessment of the injury and the athlete’s overall condition. This step helps determine whether regenerative therapy is suitable and what areas may require targeted support.
The evaluation may include:
- Review of past injuries
- Medical history and previous treatments
- Sport-specific activity analysis
- Physical examination
- Range of motion and strength testing
- Biomechanical assessment
- Review of MRI, ultrasound, X-ray, or previous reports
- Assessment of training load and recovery habits
- Risk-benefit evaluation
Step 2: Specialist Consultation
After the evaluation, patients receive a consultation where treatment options, expected recovery timelines, possible outcomes, limitations, pricing, and rehabilitation goals are explained clearly.
This consultation helps athletes understand whether regenerative therapy is appropriate and what results are realistic for their injury type.
Step 3: Stem Cell Preparation
If treatment is approved, high-quality stem cells are prepared under controlled laboratory conditions. Preparation may vary depending on the protocol, availability, and quality control requirements.
Quality control may include:
- Viability testing
- Sterility and contamination screening
- Identity confirmation
- Quality documentation
- Protocol-specific preparation
- Safety review before administration
Patients should receive clear information about the cell source, preparation process, product documentation, and expected timing before treatment day.
Step 4: Treatment Day
On the treatment day, the patient’s current condition is reviewed. The treatment area is prepared under sterile conditions, and the regenerative protocol is applied according to the personalized plan.
The treatment method may include:
- Targeted local injection for tendon, ligament, muscle, joint, or soft tissue injuries
- Image-guided application in selected cases
- PRP-supported application when appropriate
- Exosome-supported therapy when included in the protocol
- IV infusion only when medically justified and suitable
The method depends on diagnosis, injury location, tissue type, and medical suitability. Most protocols are minimally invasive, but all procedures carry potential risks and require proper aftercare.
Step 5: Follow-Up and Rehabilitation Support
Recovery does not end after the procedure. Follow-up and rehabilitation are essential for long-term success. Stemcell Consultancy provides structured guidance to help patients return to activity safely.
Follow-up may include:
- Pain and swelling tracking
- Range of motion assessment
- Strength and performance monitoring
- Rehabilitation progression
- Return-to-training guidance
- Imaging follow-up when appropriate
- Load management recommendations
- Reinjury prevention planning
Regenerative therapy works best when combined with a structured rehabilitation program and gradual return-to-sport plan.
Return-to-Sport Planning After Regenerative Therapy
Returning to sport too early may increase the risk of reinjury. A safe return-to-sport plan should be based on objective function rather than only pain reduction.
Important return-to-sport criteria may include:
- Minimal or no pain during sport-specific movement
- Full or near-full range of motion
- Restored strength compared with the uninjured side
- Good balance and neuromuscular control
- Ability to tolerate progressive training load
- No significant swelling after activity
- Successful completion of sport-specific drills
- Medical and rehabilitation team approval
Athletes should return gradually through phases such as basic mobility, strength training, controlled drills, sport-specific movement, partial training, full training, and competition readiness.
Potential Benefits of Stem Cell Therapy for Sports Injuries
Stem cell therapy may offer supportive benefits for selected sports injury patients. Individual results vary and should be monitored carefully.
Potential benefits may include:
- Support for inflammation regulation
- Reduced pain burden in selected patients
- Support for tendon, ligament, muscle, or cartilage repair signaling
- Improved movement comfort
- Better joint or soft tissue environment
- Support for collagen remodeling
- Improved rehabilitation tolerance in selected cases
- Potential quality-of-life and activity support
- Reduced recurrence risk when combined with biomechanical correction
These benefits are potential outcomes and should not be interpreted as guaranteed results, guaranteed faster return to sport, or guaranteed performance enhancement.
Who May Be a Suitable Candidate?
Stem cell therapy may be considered only after detailed medical evaluation. It is not automatically suitable for every sports injury.
Potential candidates may include individuals who:
- Have chronic tendon, ligament, muscle, cartilage, or joint injury
- Have not achieved sufficient improvement with conservative care
- Have mild to moderate tissue damage without urgent surgical indication
- Have persistent pain, inflammation, or functional limitation
- Are recovering from selected orthopedic procedures with surgeon approval
- Have realistic expectations about supportive outcomes
- Are medically stable for a regenerative procedure
- Are willing to follow rehabilitation and load management guidance
- Can attend follow-up monitoring
The best candidates are usually patients with a clear diagnosis, stable medical condition, appropriate imaging findings, measurable functional goals, and commitment to rehabilitation.
Who May Not Be Suitable?
Stem cell therapy may be postponed or avoided when risks outweigh potential benefits or when another treatment is more urgent.
Patients may not be suitable if they have:
- Unclear diagnosis
- Complete tendon or ligament rupture requiring surgical evaluation
- Severe joint instability
- Advanced bone-on-bone arthritis with major deformity
- Active infection
- Suspected joint infection
- Open wound near the treatment area
- Active cancer or certain cancer histories
- Severe uncontrolled diabetes
- Severe uncontrolled autoimmune disease
- Blood clotting disorders
- Use of blood thinners that cannot be safely managed
- Recent major surgery without clearance
- Pregnancy or breastfeeding
- Unrealistic expectations of guaranteed healing or immediate return to competition
In these cases, orthopedic evaluation, infection treatment, surgical consultation, medical stabilization, or alternative rehabilitation planning may be needed first.
Safety and Possible Side Effects
Regenerative therapy for sports injuries should be performed only after proper diagnosis and medical evaluation. Safety depends on patient selection, product source, laboratory quality, sterility testing, application method, imaging guidance when used, dose, and follow-up care.
Possible temporary effects may include:
- Mild soreness at the application site
- Temporary swelling or sensitivity
- Bruising
- Short-term increase in local discomfort
- Temporary stiffness
- Fatigue in some patients
- Rare infection, bleeding, allergic, or inflammatory reaction risk
Patients should seek medical attention if they experience fever, spreading redness, severe swelling, severe pain, pus, allergic reaction, chest pain, shortness of breath, new weakness, numbness, or unexpected worsening after treatment.
Recovery Timeline and Expectations
Recovery after regenerative therapy varies depending on the injury, tissue type, severity, athlete age, training load, rehabilitation quality, and overall health. Stem cell therapy does not usually work like an immediate painkiller. Tissue repair signaling and remodeling take time.
A general timeline may include:
- First few days: Mild soreness, swelling, or sensitivity may occur.
- First 2-6 weeks: Some patients may notice reduced pain, improved comfort, or easier movement.
- 6-12 weeks: Strength, mobility, and training tolerance may improve more clearly in selected patients.
- 3-6 months: Tissue remodeling, sport-specific function, and performance readiness may continue to develop with rehabilitation.
- Long-term follow-up: Continued strength, mobility, and load management are important to reduce recurrence risk.
Progress should be evaluated through pain scores, strength testing, range of motion, sport-specific function, swelling response, training tolerance, and medical follow-up.
Rehabilitation After Stem Cell Therapy
Rehabilitation is essential after regenerative therapy. Biological support alone is not enough if the athlete returns to poor mechanics, weak muscles, or excessive training load.
Rehabilitation may include:
- Early mobility and swelling control
- Progressive strengthening
- Flexibility and range of motion work
- Neuromuscular control training
- Balance and proprioception exercises
- Sport-specific movement retraining
- Gradual load progression
- Gait or running mechanics correction
- Jumping, landing, cutting, or throwing mechanics when relevant
- Recovery and conditioning planning
The rehabilitation plan should be personalized according to injury type, sport, performance level, competition schedule, and physician recommendations.
How to Reduce Reinjury Risk
Long-term success depends on correcting the factors that caused or contributed to the injury. Pain relief alone does not mean the tissue is ready for full competition.
Helpful reinjury prevention strategies include:
- Gradual training progression
- Proper warm-up and cool-down routines
- Strengthening weak muscle groups
- Improving flexibility and mobility
- Correcting running, jumping, landing, or throwing mechanics
- Maintaining adequate recovery between sessions
- Optimizing sleep and nutrition
- Using appropriate footwear and equipment
- Avoiding sudden increases in training volume
- Monitoring pain, swelling, and fatigue
- Continuing maintenance exercises after return to sport
A personalized prevention plan should be based on the athlete’s sport, injury history, movement pattern, training schedule, and performance goals.
Questions to Ask Before Sports Stem Cell Therapy
Before beginning treatment, patients should receive clear answers to important questions.
- What is my exact diagnosis?
- Is my injury acute, chronic, or overuse-related?
- Do I need surgery or urgent orthopedic care?
- Is stem cell therapy appropriate for my injury?
- Is the treatment approved, investigational, or protocol-based in my situation?
- What cell source will be used?
- What sterility and viability tests are performed?
- Will PRP or exosomes be included?
- Will image guidance be used?
- What benefits are realistic for my condition?
- What risks should I understand?
- How will progress be measured?
- What rehabilitation plan should I follow?
- When can I safely return to training or competition?
These questions help athletes make informed decisions and avoid unrealistic treatment expectations.
Why Choose Stemcell Consultancy for Sports Stem Cell Therapy?
Stemcell Consultancy offers personalized regenerative treatment planning for athletes and active individuals seeking advanced supportive options for sports injuries. The approach focuses on careful diagnosis, safety, transparent communication, quality-focused preparation, and long-term rehabilitation support.
Key advantages include:
- Personalized injury evaluation
- Review of imaging, medical history, and performance goals
- Customized protocols for each athlete
- MSC, PRP, exosome, and growth factor-supported options when medically appropriate
- Quality-focused laboratory preparation standards
- Image-guided application planning in selected cases
- Minimally invasive treatment approach
- Transparent explanation of benefits and limitations
- Follow-up programs for long-term recovery support
- Rehabilitation and return-to-sport guidance
- Multilingual assistance and transportation support when available
The goal is to help athletes recover responsibly, reduce reinjury risk, and return to activity with better movement quality and confidence.
Frequently Asked Questions About Stem Cell Therapy for Sports Injuries
Can stem cell therapy cure sports injuries?
Stem cell therapy should not be described as a guaranteed cure. It may support inflammation regulation and tissue repair signaling in selected injuries, but results vary depending on diagnosis, injury severity, rehabilitation, and overall health.
Can stem cell therapy help athletes return to sport faster?
Faster return to sport cannot be guaranteed. Recovery depends on tissue healing, strength, mobility, sport-specific readiness, and medical clearance. Returning too early may increase reinjury risk.
Is stem cell therapy suitable for ligament injuries?
Selected partial ligament injuries may be evaluated. Complete ligament ruptures or severe instability may require orthopedic surgical consultation.
Can stem cell therapy help tendon injuries?
Selected chronic tendon injuries may be evaluated, especially when conservative care has not provided sufficient improvement. Rehabilitation and load management remain essential.
Can stem cells regenerate cartilage?
Complete cartilage regeneration cannot be guaranteed. Stem cell therapy may support joint environment and repair signaling in selected cases, but advanced cartilage loss may require orthopedic evaluation.
Can PRP be combined with stem cell therapy?
PRP may be combined with stem cell therapy in selected cases to support tissue repair signaling. The decision depends on injury type, tissue condition, and physician recommendation.
Are exosomes used for sports injuries?
Exosomes may be discussed in selected regenerative protocols because of their role in cellular communication and inflammation modulation. Their use should be evaluated individually and explained transparently.
Is the procedure painful?
The procedure is generally minimally invasive. Some patients may feel pressure, soreness, or temporary sensitivity. Comfort measures may be used when appropriate.
How long does recovery take?
Recovery varies by injury type and severity. Some patients may notice improvement within weeks, while tissue remodeling and return-to-sport readiness may require several months.
Do I still need physical therapy?
Yes, in most cases. Physical therapy helps restore strength, mobility, neuromuscular control, sport-specific mechanics, and confidence. It is essential for reducing reinjury risk.
Can stem cell therapy replace surgery?
Not always. Some injuries require surgery, especially complete ruptures, severe instability, fractures, or mechanical joint problems. Regenerative therapy should be evaluated case by case.
Who should avoid this treatment?
Patients with active infection, unclear diagnosis, complete rupture requiring surgery, severe instability, active cancer, blood clotting disorders, pregnancy, or unrealistic expectations may not be suitable.
What should athletes track after treatment?
Athletes should track pain, swelling, range of motion, strength, training tolerance, sleep, fatigue, sport-specific performance, and any side effects. Sudden worsening should be reported to a healthcare professional.
Start Your Advanced Sports Rehabilitation Journey
Sports injuries can affect performance, confidence, daily movement, and long-term athletic participation. Because injuries may involve muscles, tendons, ligaments, cartilage, joints, biomechanics, and training load, treatment should be personalized and comprehensive.
Stem cell therapy is being explored as a supportive regenerative option for selected sports injuries because of its potential role in inflammation modulation, tissue repair signaling, cellular communication, and joint or soft tissue environment support. However, it should always be approached with realistic expectations, accurate diagnosis, medical supervision, and a structured rehabilitation plan.
Stemcell Consultancy provides individualized evaluation, regenerative treatment planning, and follow-up support for eligible athletes and active individuals seeking advanced supportive options for sports injury recovery.
Patients interested in stem cell therapy for sports injuries can contact Stemcell Consultancy to schedule a personalized evaluation and learn whether a regenerative protocol may be suitable for their recovery and performance goals.
This content is for informational purposes only and does not replace medical diagnosis, orthopedic care, sports medicine evaluation, physical therapy, emergency treatment, or professional medical advice. Sports injuries may have different causes and severity levels, and every patient should be evaluated individually by qualified healthcare professionals. Stem cell, PRP, exosome, and other regenerative approaches may not be suitable for everyone, and outcomes can vary depending on diagnosis, injury severity, tissue quality, medical history, treatment protocol, rehabilitation, training load, and follow-up care.

